Major Depressive Disorder (MDD) is a common mental illness affecting about 121 million people worldwide, and one of the leading causes of disability. The main goals of treating BDD are to achieve symptomatic remission and restore normal functioning. Despite the availability of various types of drugs that can ensure the effectiveness and tolerability of treatment, less than 25% of patients with MDI receive adequate therapy, which impedes the achievement of these goals. A. Fagiolini et al. in the article “Rediscovering Trazodone for the treatment of major depressive disorder”, published in the journal CNS Drugs (2012; 26: 1033-1049), cited data on the effectiveness of trazodone in the treatment of MDD and related diseases, as well as its use in insomnia and anxiety syndrome .
First-line treatment of moderate or severe form of BDD includes antidepressant monotherapy (AD), evidence-based psychotherapy, and / or a combination of both treatment approaches. Patients with severe forms of BDD may require the combined treatment of blood pressure and an antipsychotic, electroshock therapy, or the combined use of blood pressure and psychotherapy. Moreover, treatment strategies for patients who have not responded adequately to taking first-line drugs include switching to monotherapy with another drug, combination treatment using a different blood pressure, or using another drug to supplement the main one.
More than 20 years have passed since the advent of the AD class of selective serotonin reuptake inhibitors (SSRIs), which are widely used at present. Since then, it has been found that SSRIs and their derivatives, serotonin and norepinephrine reuptake inhibitors (SSRIs) and norepinephrine reuptake inhibitors (NRI), are comparable in effectiveness and also more acceptable in use than earlier generations of drugs, such as tricyclic antidepressants (TCAs) and monoamine oxidase inhibitors (iMAOs). However, there are significant restrictions on the use of these drugs, including low rates of achievement of remission (usually <50% for both classes of drugs, both for SSRIs and for social protection, relatively slow onset of action and the lack of stable effectiveness in general for all manifestations of depressive symptoms (Machado et al., 2006; Trivedi et al., 2006; Nierenberg et al., 1999) .This is also associated with common side effects such as sexual dysfunction, weight gain / decrease, insomnia or daytime sleepiness. as well as anxiety or irritability (Clayton et al., 2002; Fava et al., 2000, 2002, 2004, 2007; Thase, 2006).
Trazodon * is an antagonist of serotonin receptors and an inhibitor of serotonin reuptake (AIOS) and is used to treat MDD with disturbing symptoms or their absence. The drug, as a rule, is well tolerated, has fewer anticholinergic effects than imipramine and amitriptyline, and also has an antidepressant effect comparable in effectiveness to second-generation blood pressure. Trazodone is approved for sale in many countries around the world in such forms of release as immediate release tablets (TNVs), controlled release tablets (TKVs), and in some countries even as drops for oral administration and injection.
Recently, a new form of trazodone release has been developed – Contramid trazodone, once-daily sustained-release tablets (150 and 300 mg tablets, which are divided in half), created according to Contramid technology (manufactured by Angelini Labopharm LLC, Princeton, NJ, USA ) This patented technology can control the release of trazodone within 24 hours; It was developed with the aim of trying to better adhere to the patient’s treatment regimen and regimen, while maintaining efficacy and improving drug tolerance.
Due to its combined action of antagonizing serotonin receptors and inhibiting serotonin reuptake, trazodone has also demonstrated unique therapeutic flexibility, which has led to its potential use in the treatment of a wide range of concomitant diseases associated with BJD, as well as for its use other than direct indications, such as in the treatment of insomnia, anxiety, dementia, Alzheimer’s disease, drug dependence, schizophrenia, bulimia and fibromyalgia.
A literature search was conducted at the US National Library of Medicine, PubMed / MedLine, using the keywords “trazodone” and “major depressive disorder” as free text. The search came down to fully published randomized controlled trials, which were presented in English only. Each work was evaluated according to relevance, only articles published after 1981 (date of approval of the use of trazodone in the USA) were included in the test. The search for the use of trazodone not according to direct indications, including the treatment of insomnia and anxiety syndrome, was carried out separately. However, only published randomized controlled trials were considered.
Mechanisms of action and pharmacological properties of trazodone
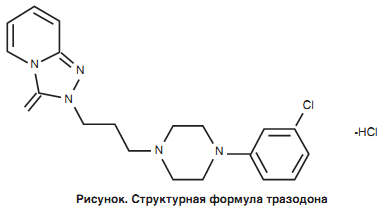
Trazodone is a derivative of triazolopyridine (figure). Although its pharmacological effect in the human body has not been fully studied, it is believed that trazodone has more than one mechanism of therapeutic action, which makes it a multifunctional drug.
Trazodone is the first AD that has a dual mechanism of action: it inhibits the serotonin transporter protein and is an antagonist of type 2 serotonin receptors (5-HT2; blocks both 5-HT2A and 5-HT2C receptors).
Preclinical data indicate that the antidepressant activity of SSRIs and SSRIs is most likely carried out by blocking the serotonin transporter protein, which leads to the agonistic effect of serotonin on 5-HT1A receptors. However, serotonin also acts on other subtypes of serotonin receptors, namely the 5-HT2A and 5-HT2C receptors, which are thought to underlie the development of side effects commonly associated with treatment for SSRIs and SSRIs, such as insomnia, sexual dysfunction, and the anxiety component . Unlike SSRIs and SSRIs, AIOS, for example trazodone, provide simultaneous inhibition of the serotonin transporter protein and also have an antagonistic effect on 5-HT2A and 5-HT2C receptors, which avoids undesirable effects associated with the activation of 5-HT2A / 2C- receptors. Moreover, there is an assumption that the simultaneous antagonistic effect on 5-HT2A / 2C receptors and inhibition of the serotonin transporter protein can give a synergistic effect that enhances the antidepressant activity of AEOS and improves treatment tolerance.
At the same time, trazodone exhibits antagonistic properties against a1- / a2-adrenergic receptors and H1-histamine receptors, as well as a slight anticholinergic effect. It is also well known that in small doses (25-100 mg), trazodone has a hypnotic therapeutic effect. As is known, several neurotransmitter systems are involved in the excitation mechanism, including serotonin, norepinephrine, dopamine, acetylcholine and histamine. Thus, by suppressing the activity of some of these neurotransmitter systems, it is possible to effectively inhibit the excitation process and activate the sleep process. The effectiveness of trazodone in this regard can be explained by its ability to inhibit H1 receptors, and the hypnotic effect due to blockade of such receptors can be enhanced by antagonistic effects on both 5-HT2A receptors and a-adrenergic receptors.
According to a brief description of the drug, trazodone therapy should begin with an evening dose (initial dose – 75-150 mg at bedtime). Subsequently, the dosage can be increased every three days to 300 mg / day by introducing repeated doses after meals (for TNV), two or once a day, preferably at night (for TKV). For inpatients, the dosage can be increased to 600 mg / day by repeated doses. For the elderly, the initial dose should be reduced to 100 mg / day.
Controlled-release trazodone
75 and 150 mg controlled-release trazodone tablets were developed in the 1980s. in order to limit the early and relatively high peak plasma concentrations of the drug, which is observed when taking tablets with immediate release. This high peak in plasma concentration may be associated with the occurrence of side effects, such as drowsiness or hypotension, especially in the first weeks of treatment. These adverse events can affect the tolerance of treatment and adherence to its regimen, which in turn limits the use of a therapeutic dose (up to 300 mg / day) in patients with depression.
As reported in the brief description of the drug, after ingestion of a single dose of 100 mg of TNV, the maximum concentration of the drug in plasma (Cmax) of 1.2 mg / ml is achieved with the time necessary to achieve its maximum concentration in plasma (Tmax) – 1 hour. For the form of trazodone, TKV after a single oral dose of 75 mg of Cmax is about 0.7? G / ml and is reached within a time of Tmax of 4 hours. After ingestion of a single dose of 150 mg of TKV Cmax, which is about 1.2 mg / ml, is achieved during Tmax – 4 hours after administration. The half-life is about 12 hours.
The recently approved form of the extended-release drug Contramid should further ensure the optimal intake of this blood pressure and may be useful for prescribing appropriate therapeutic doses and better patient compliance with the treatment regimen and regimen.
Trazodone in the treatment of BDR
Approved for use, trazodone showed antidepressant activity comparable to other classes of drugs, such as TCAs, SSRIs, and SSRIs in several clinical studies. Thus, trazodone can be prescribed in the form of monotherapy or in combination treatment with other blood pressure in patients with BDD.
Despite the proven effectiveness and popularity of blood pressure in the United States during the 1980s, current treatment guidelines suggest that currently in the United States TNVs are more likely to be used in lower doses as sedatives / hypnotics than HELL. However, limited clinical evidence exists to support the use of trazodone for this indication, and in the United States, as well as in most countries around the world, they continue to approve the use of trazodone solely for the treatment of depressive disorders.
Efficacy and tolerability of trazodone
Several direct comparative studies have demonstrated the effectiveness of blood pressure comparable between trazodone and drugs of other classes – TCA (amitriptyline and imipramine), SSRIs (fluoxetine, paroxetine, sertraline, citalopram and escitalopram), SSRIs (venlafaxine and mirtazaporin naphtha and dopamine (bupropion). Table 1 shows the results of randomized controlled clinical trials of trazodone conducted after 1981 in patients with BDR.